You’ve probably come across the name on a blog, a social post, or a search result. Maybe a colleague mentioned it. But when you look for hard details — who runs it, where it’s registered, what real providers say — the trail goes quiet fast. Every page describing how Care Qevafaginz Network Ltd works for providers reads almost identically, which is itself worth noticing.
For this guide, we compared those public descriptions side by side, checked basic business information where available, and mapped the claims against standard expectations for healthcare IT platforms rather than relying on any single promotional source.
So here’s what this guide actually does. It walks through what the platform claims to offer providers, what those claims mean in practical workflow terms, and — critically — what you should verify before sharing a single byte of patient data with any healthcare platform you can’t independently vet. The features described across the web are real healthcare IT needs. Whether this specific platform delivers on them the way it claims is a question only direct due diligence can answer.
This guide is for practice managers, clinic administrators, and healthcare providers who want a straight picture, not a sales pitch.
Table of Contents
What You Need to Know
- Care Qevafaginz Network Ltd is described across multiple sources as a healthcare operations platform connecting providers, patients, and insurers — but its registration and credentials cannot be independently verified through public company records.
- Claimed features include administrative automation, EHR integration, billing management, telehealth tools, and secure data transfer.
- The platform is presented as a connector layer that works alongside your existing systems rather than replacing them.
- Before joining any platform like this, providers should request a Business Associate Agreement, ask about specific EHR compatibility, and confirm compliance certifications.
- This guide covers claimed features, workflow implications, data security considerations, and a due diligence checklist you can use for any platform evaluation.
What Is Care Qevafaginz Network Ltd?
Care Qevafaginz Network Ltd is described across its website and third-party sources as a cloud-based healthcare coordination platform designed to help medical providers manage administrative workflows, connect with patients and insurers, and exchange data securely. According to its own website, it acts as a connector between existing systems rather than a replacement for them — the idea being that your current EHR and practice management tools stay in place while the platform adds a coordination layer on top.
Snapshot definition (40–60 words, snippet-ready): Care Qevafaginz Network Ltd is described as a healthcare operations platform that connects providers with patients, insurers, and administrative systems through a centralized digital interface. It claims to automate scheduling, billing, and data exchange while integrating with existing EHR software — though its company registration and independent compliance certifications have not been publicly verified.
That last part matters. The SERP for this keyword is dominated by very similar content from low‑authority blogs, many of which read like near‑copies of the same underlying narrative. There are no independent reviews from verified healthcare providers, no press coverage from healthcare IT publications, and no visible regulatory filings. That doesn’t mean the platform doesn’t exist or doesn’t function — but it does mean every feature claim should be treated as stated, not proven, until you verify it directly.
For providers in Pakistan, that step of the verification process should also consider local laws at a minimum. You‘re probably best off finding out how the platform purports to treat data under Pakistan‘s Prevention of Electronic Crimes Act, what sector-specific health data guidance from regulators is in effect in the country, and which country‘s laws generally apply to the vendor‘s cloud network.
How Does the Provider Onboarding Process Work?

Getting started. That’s usually the first real question — and the first place where the gap between marketing language and operational reality tends to show up.
In the onboarding model as described in the platform, providers credentials are verified before completing registration. Providers usually upload their licensing, practice information and qualification documents via secure online portal. After their credentials have been verified, providers are given access to their custom dashboard which allows them to manage their network activity.
Credentialing and Registration
The credentialing step is described as thorough but efficient. Providers submit their professional licenses, specialty credentials, and practice information. The platform claims to verify this information before granting full access — a standard approach for any legitimate healthcare network.
What you should ask directly: How long does credential verification take? Who conducts the verification? Is there a third-party credentialing service involved, or is it handled internally? These aren’t trick questions — they’re standard due diligence for any provider network you’re joining.
Training and Dashboard Setup
After credentialing, the onboarding model described includes role-specific training. Clinical staff are said to focus on patient management and documentation tools, while administrative staff cover billing and scheduling. Managers get access to analytics and reporting features. According to one source, most small‑to‑medium practices are described as reaching operational readiness within one to two weeks, but there are currently no independent case studies or verified provider reviews available to confirm that timeline.
That’s plausible for a well-designed platform. But it does depend on how complex your existing setup is — and whether the platform’s integration with your specific EHR is pre-built or requires custom configuration.
What Administrative Functions Does the Platform Handle?
Here’s where the clearest provider value is claimed — and where the features described align with real, documented pain points in healthcare operations.
Administrative burden is one of the most consistently documented problems in provider satisfaction data. According to AMA survey research, physicians in 2024 reported spending 7.3 hours per week on administrative tasks — separate from direct patient care — with billing, prior authorization, and documentation driving the bulk of that load. So the appeal of a platform that claims to automate these functions is legitimate, regardless of the specific vendor.
Common admin pain points vs. what platforms like this claim to fix
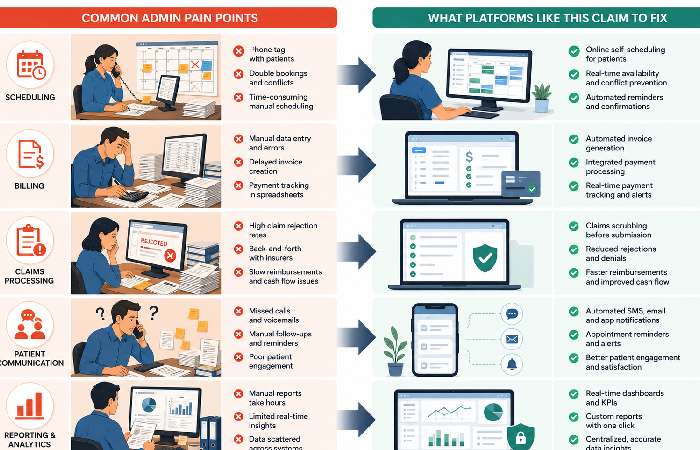
| Pain point in a typical practice | How platforms like this say they help |
|---|---|
| Phone‑based scheduling and constant rescheduling | Online booking, automated reminders, and rules for handling no‑shows |
| Manual coding and error‑prone claims submission | Built‑in coding suggestions and electronic claim submission to payers |
| Spreadsheets for tracking receivables and revenue | Dashboards showing charges, payments, denials, and aging by payer |
| Staff time spent chasing unpaid balances | Automated statements, payment links, and follow‑up reminders to patients |
Scheduling and Appointment Management
The platform is described as automating appointment scheduling, including patient booking, reminder notifications, and follow-up triggers. Providers can reportedly set preferences for notification types and customize workflows around their scheduling patterns. Smart routing is mentioned — when a referral comes in, it’s described as automatically directed to the appropriate department or specialist without manual handoff.
In practice, how much this feature is depends on two factors: whether your scheduling software can be plugged into your baseline calendar, and whether paitents have the option to book without staff intervention. Both are worth double checking before you bank on them.
Billing, Claims Processing, and Insurance Integration
This is described as one of the platform’s core functions. According to multiple sources, the system automates billing submissions, tracks claims in real time, handles patient copays and deductibles, and generates financial reports for revenue cycle management. Automated invoicing is said to reduce billing errors and speed up payment cycles.
Billing automation in healthcare IT is a real and well‑documented efficiency gain in general; American Medical Association research on administrative burden shows billing and prior authorization consume a significant portion of physician time, even though that data does not refer to Care Qevafaginz Network Ltd specifically. If this platform genuinely integrates with your payer networks and automates clean claim submission, that’s meaningful. But the critical question — which payer networks, and which insurance systems specifically — is something you’d need to confirm with the platform directly, not from a third-party blog.
How Does EHR and System Integration Work?
“Works with your existing systems.” You’ll see that phrase on nearly every page describing this platform. It’s a common and appealing claim in healthcare IT. But it means different things depending on your setup.
The real EHR integration would involve native API connections to the various EHR platforms, or being compatible with a common standard for interoperability, such as, HL7 FHIR, the open APIbased standard (maintained by HL7, and supported by the ONC) defining how health information should be structured and communicated in order to transfer between different systems. TheOffice of the National Coordinator for Health IT (ONC) has put in place interoperability requirements that certified health IT systems in the U. S. Will have to meet.
If a platform claims to integrate with your EHR, asking whether it uses HL7 FHIR‑compliant data exchange is a reasonable and specific question. Even if your practice is outside the United States, ONC’s interoperability rules and HL7 FHIR‑based approaches are still useful benchmarks for what modern, standards‑aligned integration should look like, even when your own regulator uses different terminology.
The platform’s described integration approach positions it as an intelligent coordination layer — connecting to EHR platforms, practice management software, laboratory systems, and medical device networks without requiring organizations to abandon their existing tools.
| Claimed Integration Capability | What to Verify Before Relying on It |
|---|---|
| Connects with existing EHR systems |
Which specific EHR platforms? Is it pre‑built or custom? |
| Integrates with payer/insurance networks | Which payers? Does it support EDI 837 claim submissions? |
| Laboratory and imaging system connectivity | Via which standards? HL7 v2, FHIR, or proprietary? |
| Medical device / wearable data sync | Which devices? Is data mapped to EHR fields automatically? |
| Scheduling calendar integration | Which calendar systems? Is it bidirectional? |
Three integration red flags to watch for
- The vendor cannot name specific EHRs and versions they have already integrated with.
- There is no written API or interoperability documentation you can review before signing.
- Explanations stay at buzzword level (“seamless,” “plug‑and‑play”) without describing how data is mapped, tested, and monitored in practice.
That table isn’t meant to be discouraging — it’s the kind of question any responsible IT procurement process asks. A platform that can answer those clearly is a platform worth evaluating further. One that can’t answer them clearly is one to approach with caution.
How Does the Platform Handle Data Security and Compliance?
Right. This is the section where most competing articles write the words “encryption” and “real-time threat detection” and move on. That’s not enough — not for healthcare data, and not for any provider who’s responsible for protecting patient information under the law.
What the Platform Claims About Encryption and HIPAA Alignment
Sources describing the platform consistently reference encryption, secure data transfer protocols, HIPAA compliance, and audit trail functionality. One source specifically describes automated documentation and audit trails that track every access and modification of patient data — which aligns with what the HIPAA Security Rule actually requires.
So let’s ground that in reality. As HHS’s official HIPAA Security Rule summary confirms, the Security Rule requires regulated entities to implement appropriate administrative, physical, and technical safeguards to ensure the confidentiality, integrity, and availability of electronic protected health information — and those same obligations extend to any business associate handling that data on a provider’s behalf. Under the technical safeguards framework, covered entities and their business associates must implement access controls, audit controls, integrity controls, and transmission security measures — the full scope of which is outlined in HHS’s official technical safeguards guidance. That’s the actual standard — not just “encryption,” but a documented set of controls covering access management, data integrity verification, and secure transmission.
Claiming HIPAA compliance without documentation is easy. Proving it requires an independent audit, published security certifications, or at minimum a signed Business Associate Agreement that creates legal accountability.
What Providers Should Actually Verify
Before sharing patient data with any third-party platform, including this one, these are not optional questions:
- Is there a signed Business Associate Agreement (BAA)? According to HIPAA, all vendors who will be managing your ePHI for you must be a Business Associate, and you must have a BAA before sending any protected health information to a platform. If a vendor won to provide one hard stop.
- Is the platform certified to any security standards? An independent audit framework, such as SOC2 Type II, HITRUST, or ISO 27001, confirms the existence of security controls. Don‘t be afraid to ask it‘s common practice.
- Where is data stored? How the cloud and it’s data is located is equally serious issues and cloud region, data residence and backup plans matter both from compliance and disaster recovery prospective.
- How is breach notification handled? Under HIPAA‘s Breach Notification Rule, covered entities must be notified within 60 days of discovery of a breach. Your BAA should state this.
If you practice outside of the United States and are not directly subject to HIPAA, these controls can provide a handy cost-effective starting point against which to measure an administration, technical, and physical safeguard standard you should expect from a vendor that cannot describe how its controls meet the benchmarks of these more fundamental expectations.
None of this is meant to imply the platform fails these checks. It’s that no publicly available source confirms it passes them — and the burden of verification sits with you, not with a blog post.
What Patient Engagement and Telehealth Tools Are Offered?
Telehealth is no longer a trade-only feature. It‘s here to stay, and the supporting technologies range from extremely effective and compliant to poorly designed and difficult to use.
Communication and Messaging Features
The site is said to be a secure messaging system between providers and patients for between visit communications, automated appointment reminders, follow-up instruction, and health education content delivery. Patient portals are said to be available, providing access to patient records, appointment history and patient wellness information.
And honestly, these features are table stakes for any modern practice management platform. The differentiator isn’t whether they exist — it’s whether they’re easy enough that patients with limited tech familiarity can actually use them. That’s the part you’d need to evaluate through a demo or trial period.
Telehealth and Remote Monitoring Claims
Video consultation features, remote patient monitoring data uploading from wearable devices, copying the telemedicine visit into the Electronic Medical Record (EMR), and eprescription generation during the virtual visit, are all mentioned in platform-specific sources, but there has been no independent testing or third-party sources publicly available to demonstrate how well they actually perform in real-world clinics. For healthcare providers serving remote or underserved patient population, or homebound patients, if these features work remotely as they are said to do, they can truly increase the scope of care delivered at no extra expense.
The qualification there is important. Remote monitoring integration, in particular, depends on which devices are supported and whether data flows automatically into patient records or requires manual reconciliation. That’s a workflow question with real clinical implications.
When you test telehealth features in a demo, try to:
- Join a visit from a low‑bandwidth or mobile connection to see how the system handles poor networks.
- Have a non-technical staff member participate in a test session with just the directions sent by the platform.
- Make sure where the visit recordings (if any), chat logs and eprescriptions are being saved and for how long, and who has access to these records.
- These simple stresstests reflect what many IT and clinical leaders will attempt when temporarily providing remote care using a telehealth platform, and can identify whether a tool is truly ready for the realities of their network and their patients.
What Should Providers Verify Before Joining Any Platform Like This?
This kind of section — focused on what to verify rather than what a vendor claims — is largely missing from the current SERP. It is also the part of an evaluation that actually protects you.
Whether you’re evaluating Care Qevafaginz Network Ltd or any other healthcare coordination platform you’ve found through a search, the following five checks should happen before you sign anything or share patient data.
5‑point due‑diligence checklist (at a glance)
- Confirm the legal entity and registration details.
- Get a signed BAA or equivalent data‑processing agreement.
- Verify specific EHR and system compatibility in writing.
- Review independent security certifications or audit evidence.
- Speak to at least one current provider using the platform.
How to document your vendor evaluation
As you collect these answers, record them in a simple comparison sheet for all vendors you are considering. That makes it much easier to justify a final choice internally based on documented evidence instead of whoever delivered the most polished demo.
1. Confirm legal entity registration. A legitimate healthcare technology company should be findable in a public company registry. In Pakistan, that means the Securities and Exchange Commission of Pakistan (SECP) company search. In the UK, Companies House. In the US, state business registries. If you can’t locate the company’s registration, ask them directly for their registration number and jurisdiction.
2. Request a Business Associate Agreement before any data sharing. As noted above, this is a legal requirement under HIPAA for any vendor handling ePHI. No BAA, no data sharing. Full stop.
3. Request specific EHR compatibility documentation. “Integrates with most major EHRs” isn‘t the same as “integrates with [your particular EHR version].” Have it in writing and find out if this integration (if you need it) is an out-of-the-box solution or something that needs to be built.
4. Request independent security certifications or audit reports. SOC 2 Type II is the most common. HITRUST is the most rigorous in healthcare. If neither exists, ask what security assessment process the platform has undergone and who conducted it.
5. Talk to a current provider on the platform — not a case study, a real conversation. Any platform with a genuine provider base should be able to connect you with reference users. If they can’t or won’t, that’s worth noting.
Who Is This Platform Best Suited For — and Who Should Proceed with Caution?
Not every platform fits every practice. And no honest guide about a tool like this should skip this question.
Use the table below as a sense‑check for fit. It does not endorse Care Qevafaginz Network Ltd; it simply helps you think about whether your practice profile matches the type of organization these claims appear to target.
| Best suited for | Proceed with caution if |
|---|---|
| Multi-provider clinics managing disconnected admin systems | You’re a solo practitioner with minimal admin overhead |
| Practices exploring telehealth without building separate infrastructure | Your EHR has a locked, proprietary system with limited API access |
| Organizations with high billing complexity and payer diversity | You operate in a heavily regulated environment requiring documented compliance certifications before adoption |
| Groups looking to centralize scheduling and claims in one interface | You cannot get direct, documented answers to the five verification questions above |
But here’s the thing — that second column applies equally to any new platform you evaluate, not just this one. The verification framework above isn’t punitive toward Care Qevafaginz Network Ltd specifically. It’s what responsible adoption of any healthcare technology looks like.
Frequently Asked Questions
Q: What is Care Qevafaginz Network Ltd and what does it do for providers?
A: It’s described across multiple sources as a cloud-based healthcare operations platform that connects providers with patients, insurance systems, and administrative tools. Claimed functions include scheduling automation, billing management, EHR integration, telehealth capabilities, and secure data exchange. The platform is positioned as a connector rather than a replacement for existing systems — though its company registration and independent compliance credentials aren’t publicly documented, so providers should verify those directly.
Q: How does the provider onboarding process work?
A: Credential submission first, then verification, then dashboard access. The described process involves providers submitting their licenses and practice details through a secure portal. After verification, role-specific training covers the tools relevant to each staff function. According to platform sources, most small-to-medium practices reach operational readiness within one to two weeks — though that depends on your existing setup and how complex your EHR integration turns out to be.
Q: Is Care Qevafaginz Network Ltd HIPAA-compliant?
A: Platform sources describe it as HIPAA-aligned, referencing encryption, audit trails, and secure messaging. But here’s the practical answer: “HIPAA-compliant” is a claim any vendor can make. What actually protects you is a signed Business Associate Agreement that creates legal accountability, and independent security certifications that verify controls are actually in place. HHS’s HIPAA Security Rule requires covered entities and their business associates to implement specific administrative, physical, and technical safeguards — ask the platform which of those they’ve had independently audited.
Q: Does Care Qevafaginz Network Ltd integrate with existing EHR systems?
A: The system allows you to keep your existing EHR platform your EHR system so you‘re not changing platforms. But saying the app “integrates with major EHRs” can mean a whole lot of things from a sophisticated, two-way API connection, all the way to simple data export. You should ask which versions of EHRs this integration is compatible with, if the integration supports HL7 FHIR open data standards, and if the integration needs to be built or is “out of the box.”
Q: What should providers check before joining any healthcare network platform?
A: Five things. Confirm the legal entity is registered and findable. Request a Business Associate Agreement before any data sharing — this is a legal requirement, not optional. Get written documentation of specific EHR compatibility. Ask for independent security certifications (SOC 2 Type II or HITRUST). And speak with a current provider on the platform directly, not just read case studies. Those five checks apply to any platform, not just this one.
This article is provided for informational purposes only. Nothing in this article is provided to be the legal, medical or compliance advice. The medical practitioners should always approach with appropriate legal and IT compliance professionals before selecting an implemented new platform that may be use to capture healthcare data.

